
Young adults spend 80 to 100 minutes per night in slow-wave sleep, while people over age 60 generally have less than 20 minutes. "This decrease in slow-wave sleep resembles the changes in sleep patterns caused by 40 years of aging," Tasali said. On average, however, subjects required about 250-300 interventions each night, fewer the first night but more on subsequent nights as "slow-wave pressure," the body's need for deep sleep, accumulated night after night. When asked about the sounds the next morning, study subjects vaguely recalled hearing a noise "three or four times," during the night. "Our system proved quite effective," Tasali said. This technique enabled the researchers to decrease slow-wave sleep by about 90 percent, shifting the subjects from the onset of deep sleep (stage 3 or 4) to a lighter sleep (stage 2) without altering total sleep time. These sounds were loud enough to disrupt deep sleep but not so loud as to cause a full awakening. 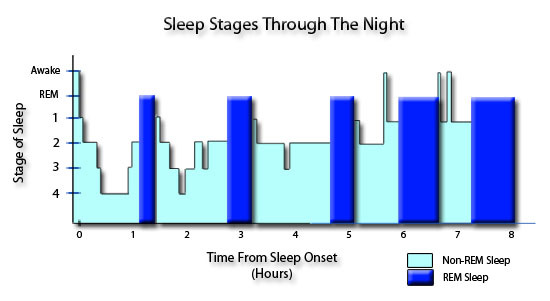
During this session, however, when their brain waves indicated that they were drifting into slow-wave sleep they were subtly disturbed by sounds administered through speakers beside the bed. 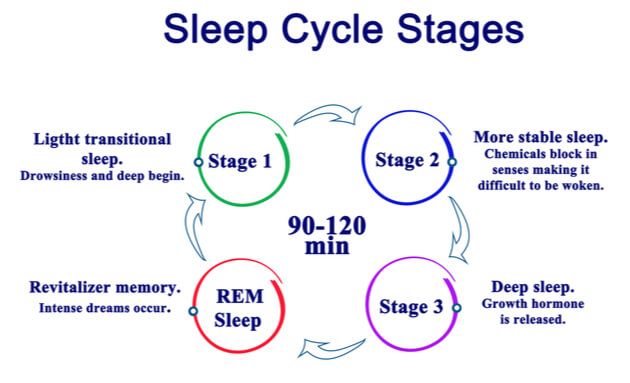
The same subjects were also studied for three consecutive nights during which they followed identical nighttime routines. The subjects spent two consecutive nights in the sleep laboratory, where they went to bed at 11 P.M., slept undisturbed but carefully monitored, and got out of bed 8.5 hours later, at 7:30 A.M. 
The researchers studied nine lean, healthy volunteers, five men and four women between the ages of 20 and 31. "Since reduced amounts of deep sleep are typical of aging and of common obesity-related sleep disorders, such as obstructive sleep apnea these results suggest that strategies to improve sleep quality, as well as quantity, may help to prevent or delay the onset of type 2 diabetes in populations at risk," said Eve Van Cauter, PhD, professor of medicine at the University of Chicago and senior author of the study. "A profound decrease in slow-wave sleep had an immediate and significant adverse effect on insulin sensitivity and glucose tolerance." "These findings demonstrate a clear role for slow-wave sleep in maintaining normal glucose control," said the study's lead author, Esra Tasali, MD, assistant professor of medicine at the University of Chicago Medical Center. This current study provides the first evidence linking poor sleep quality to increased diabetes risk. Previous studies have demonstrated that reduced sleep quantity can impair glucose metabolism and appetite regulation resulting in increased risk of obesity and diabetes. The decrease in insulin sensitivity was comparable to that caused by gaining 20 to 30 pounds. Although they needed more insulin to dispose of the same amount of glucose, their insulin secretion did not increase to compensate for the reduced sensitivity, resulting in reduced tolerance to glucose and increased risk for type 2 diabetes. This study found that after only three nights of selective slow-wave sleep suppression, young healthy subjects became less sensitive to insulin. Deep sleep, also called "slow-wave sleep," is thought to be the most restorative sleep stage, but its significance for physical well-being has not been demonstrated.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
